Share this @internewscast.com

Rosemary is now having treatment in Thailand (Image: PA Real Life)
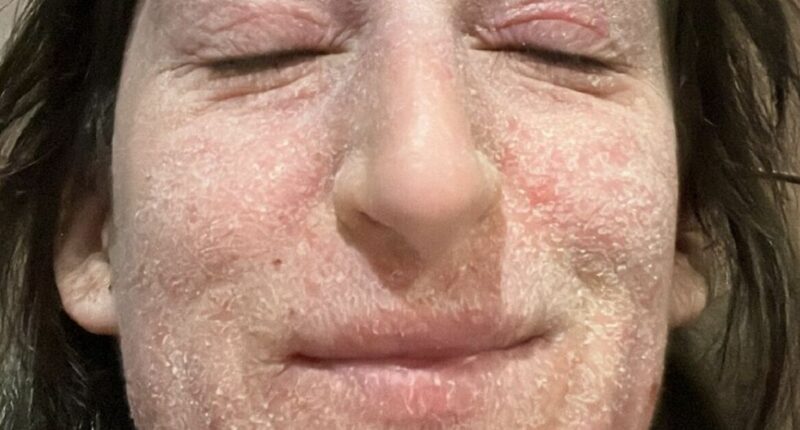
A woman has revealed she was left bedbound with “oozing”, elephant-like skin – so severe she was “unrecognisable” – after 28 years of using steroid creams for eczema, which she believes triggered topical steroid withdrawal. Rosemary Hook, 29, says she had been prescribed steroid creams for eczema since she was three months old, at increasing strengths, and claims the medication’s information leaflets advise limiting use to one week at a time.
A woman has shared her harrowing experience of being bedridden with severely inflamed, “oozing” skin resembling that of an elephant, rendering her nearly unrecognizable. This condition emerged after 28 years of using steroid creams for eczema, which she believes led to topical steroid withdrawal (TSW). Rosemary Hook, 29, explained that she has been prescribed these creams since she was just three months old, with dosage strength increasing over time. Typically, the medication’s guidelines suggest using these creams for no more than one week at a stretch.
After moving to London in 2016, Rosemary’s condition worsened dramatically. Her skin became red and inflamed all over her body, she experienced significant hair loss, and the pain was so intense it left her unable to move. Seeking answers, she turned to social media, where she discovered the concept of TSW, which she suspected was causing her symptoms to worsen and rendering her reliant on the steroid treatments.
For ten years, Rosemary struggled with skin that she described as “alien-looking,” along with depression and anxiety. Despite raising her concerns, her general practitioner dismissed them and instead prescribed immunosuppressants, including a type of chemotherapy drug, to manage her symptoms. When her condition took a turn for the worse in 2025, she traveled to Thailand in December for plasma therapy, a treatment she calls “life-changing,” as it allowed her to finally see a familiar face in the mirror again.
With each session costing £200, Rosemary now faces up to five years of ongoing treatment and has started a fundraiser to help cover the costs.
Rosemary, who works as a technician at the Bartlett School of Architecture, University College London, described her ordeal: “My skin became thickened in places, almost like an elephant’s texture, yet incredibly fragile. Deep cracks would form, and even the slightest movement could cause my skin to split or tear, which made simple tasks like getting dressed painful.”
She added, “I dealt with constant flaking and shedding throughout the day, and the persistent irritation, including areas that would ooze or bleed, was physically exhausting to manage. The changes to my appearance were so drastic that at times I didn’t recognize my own face or body, making me incredibly anxious about leaving the house or being seen by others.”
Rosemary believes she has topical steroid withdrawal (Image: PA Real Life)
Read more: Doctor explains feeling sluggish could be symptom of common condition
Read more: People with common problems ‘have 35pc higher diabetes risk’
Rosemary explained she had been prescribed steroid cream for her full-body eczema since she was three months old. Throughout the years, she received creams with progressively stronger potency, yet she said they appeared to make “much of a difference”.
When she relocated to London in 2016, her skin experienced a “big flare up”, becoming exceptionally red, painful and inflamed. Desperately seeking answers, she took control of the situation herself and discovered others on social media discussing topical steroid withdrawal – believed to be an extreme withdrawal reaction to the extended use of steroid creams.
Rosemary believes this to be the root cause of her symptoms, yet claims doctors have refused to formally diagnose her, instead prescribing immunosuppressants, including a type of chemotherapy drug. Her symptoms, such as red and inflamed skin all over her body, have persisted for the past 10 years, causing severe pain and leaving her immobile at times.
Prior to this, she described herself as “active and sporty”, with no mobility issues. Over time, her hair has fallen out in clumps, and she has struggled to carry out basic tasks such as washing and cooking. She has been bedbound on numerous occasions and has been forced to stop working for weeks at a time.
She said: “I’ve struggled with anxiety and depression – I was isolating myself so much because of the way I looked and because I wasn’t able to physically move, I was just in complete survival mode for a very long time.”
She revealed that she had attempted to stop taking her medication to observe how her skin would react, but it would “instantly” deteriorate, which she felt suggested her skin was “completely dependent” on it.

Rosemary had to stop working for weeks at a time (Image: PA Real Life)
She explained: “The rebound effects, of my skin burning and being so red, made me give in and use them again, so it was like a vicious cycle until they stopped working entirely.”
Over the years, she has consulted “countless” specialist dermatologists in London, and revealed she was “dismissed and laughed at” for voicing concerns that the steroid creams were causing further damage.
“On the labels of my creams it says that they should only be used for the maximum of one week at a time,” she said.
“GPs have told me I’m not looking after myself properly, and that I’m deliberately trying to make myself unwell. People tend to look at me in public because of my skin, and it does look quite alien at times.”
More recently, Rosemary has joined social media support groups and stumbled upon TikTok accounts where fellow sufferers share their stories under the TSW hashtag.
She said: “There are thousands and thousands of people with the same experiences as me, but it’s so under-researched and the NHS don’t really recognise the condition.”
Since summer 2025, Rosemary’s skin has deteriorated further, turning “bright red and swollen” and feeling like “elephant skin”, frequently cracking and oozing. Through her social media research last year, she discovered a clinic in Thailand offering Cold Atmospheric Plasma (CAP) therapy.
The treatment utilises ionised gas, which purportedly promotes skin healing, reduces inflammation and eliminates pathogens. She commenced treatment in Thailand in December 2025, at a cost of £200 per full-body session once a week.
She said: “It’s been amazing so far, and pretty life-changing – I can now recognise myself in the mirror. I can be fully independent again in terms of daily activities.
“My skin is getting so much stronger without any medication. There’s a long way to go – it’s easily triggered by irritants and I can’t really go anywhere here in Thailand because of the heat and the sweat.”

Rosemary has been bedbound on numerous occasions (Image: PA Real Life)
Two months of weekly sessions remain before she returns to the UK to continue treatment at a specialist clinic, where appointments will gradually become less frequent. However, her specialists estimate she will require treatment for the next five years, eventually tapering down to just a handful of sessions annually.
Her treatment has proved a “financial burden”, though her employer has permitted her to take medical leave. She has launched a fundraiser, with a target of £6,000, to assist in covering the cost of future treatments.
She added: “It would just take all of the worry away, if I met the target, and would mean I’d get my life back.”
According to the NHS website, those who have been using topical corticosteroids for an extended period should consult their doctor to review their treatment, where they may be advised to discontinue use gradually to avoid a withdrawal reaction. Those who cease using topical corticosteroids after prolonged continuous use, typically more than 12 months in adults, may experience a withdrawal reaction, which can on occasion be severe.
To donate to Rosemary’s fundraiser, visit her GoFundMe.