Share this @internewscast.com
The current surge in meningitis cases has been labeled by Meningitis Now as the most significant outbreak in the UK since the 1980s. This alarming situation has already claimed the lives of two young individuals and has affected over 20 others.
In response, the University of Kent, identified as the outbreak’s focal point, has initiated a precautionary measure by administering antibiotics to thousands of concerned students.
To combat the spread of the disease, an emergency vaccination campaign commenced on Wednesday, targeting meningitis B—the strain believed to be responsible for these cases.
This raises critical questions: What has triggered this outbreak? Should we all be vigilant for symptoms? And why isn’t the protective vaccine more commonly utilized?

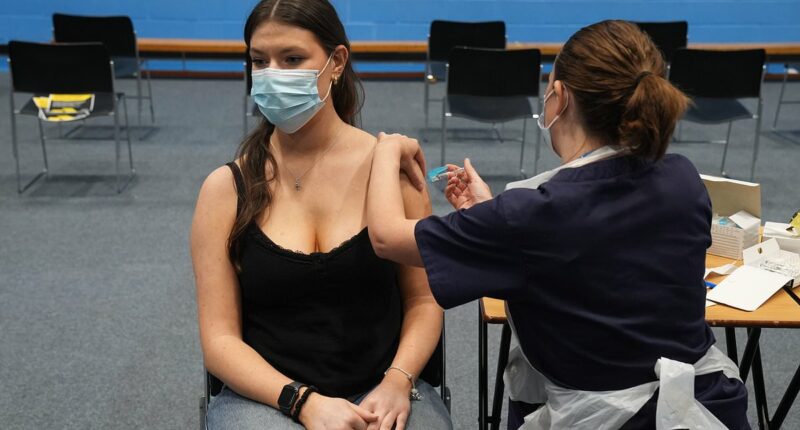
Students wait in line at the entrance to the sports hall at the University of Kent, where the rollout of a meningitis B vaccine to about 5,000 students began on Wednesday

A student receives an injection in the sports hall at University of Kent on Wednesday
What is meningitis B?
Meningitis B arises from an infection by Neisseria meningitidis group B bacteria, which targets the meninges—the protective layers enveloping the brain and spinal cord.
meninges, the protective membranes that surround the brain and spinal cord.
There are several strains of MenB, as well as other common types of bacterial meningitis – known as meningitis A, C, W and Y – as well as a less dangerous form of the infection caused by a virus.
How would I know if I had it?
Symptoms can vary and be mistaken for something much less serious, such as a cold or flu, but the NHS says the key signs to look out for are a sudden high fever, a severe headache that quickly gets worse, a stiff neck, vomiting, diarrhoea, and a dislike of bright lights.
As the infection progresses it can cause extremely cold hands and feet, shivering, severe joint and muscle pain, delirium and seizures.
When should I seek medical help?
Don’t wait for the classic rash, which is caused by bleeding under the skin as the infection rampages through the body.
If the rash doesn’t fade when you press a glass on it, it’s very likely to be meningitis. But as Mail columnist and A&E consultant Professor Rob Galloway explains, a rash is a sign that the infection has already moved from the brain into the body.
And, in some cases, there is no rash. The NHS says if you have only a few of the symptoms but still feel generally unwell, get help immediately: ‘Trust your instincts and don’t wait for all the symptoms to appear or for a rash to develop.
‘Someone with meningitis can get a lot worse very quickly.’
How does it affect your body?
The biggest risk is that the bacteria gets into the bloodstream and triggers deadly sepsis, where the immune system overreacts, leading to blood clots and a drastic drop in blood pressure. The organs then shut down rapidly.
Survivors can be left with hearing loss, poor memory and, in the most severe cases, require limb amputation. Treatment usually involves intravenous antibiotics, oxygen and steroids to reduce swelling around the brain.
Who is most at risk?
Around one in five of us carries the bug that causes MenB at the back of our throats, where it will live harmlessly and cause no health problems.
Some groups are more vulnerable, as their immune systems are not fully matured: most at risk are babies and children under five, then teenagers and young people.
Around one in four young adults aged between 15 and 19 carries the meningococcal bacteria. Research in 2010 by experts at Imperial College London suggested that our risk of infection may partly be due to genes.
Is a dangerous new strain to blame for this outbreak?
Some experts think it’s a possibility. ‘It’s likely that this will be a strain that is very slightly different from normal,’ says Adam Finn, a professor of paediatrics at Bristol University.
Another possible reason for the Kent outbreak, says Professor Finn, is ‘that this cohort of young adults infected would have been in lockdown for long periods during the Covid-19 pandemic. That means they may have less naturally acquired immunity to meningitis B because they were not regularly exposed to the bacteria.’
There has been a suggestion on social media that the outbreak is linked to Russia, where rates of the infection soared last year – but this is unproven.
Can I catch it on a crowded bus?
It’s very unlikely. Meningitis is spread by inhaling infected droplets or from direct saliva contact (for example from kissing or sharing a vape or cigarette or utensils and cutlery).
But it’s nowhere near as transmissible as the flu or Covid-19, says Andrew Lee, a professor of public health at Sheffield University.
Should we all get the vaccine?
In a programme launched in 2015, babies born in the UK are offered a MenB vaccine in three doses – at eight weeks, 12 weeks and 12 to 13 months. This covers the main subtypes of MenB but not all. It doesn’t stop the spread of the bacterium – it reduces your chances of getting seriously ill from it.
The Joint Committee on Vaccination and Immunisation – the panel that advises ministers on jabs – has previously decided not to include teenagers in the vaccination programme on the grounds that the small number of cases it might prevent didn’t justify the cost.
Since the outbreak, demand for private vaccines – costing around £200 or more – has soared. It can take several weeks for the jab to work, which means the students being immunised now could still be at risk from the current outbreak.