Share this @internewscast.com
The seemingly simple inquiry, “How are you?” may appear identical when penned on paper, but it carries distinctly different meanings. The first version is often a mere formality, prompting the expected response, “Good, thanks. How about you?” It serves as a polite exchange where a detailed answer is rarely anticipated. In contrast, the second version is something the NHS must refine if personalized cancer plans are to truly succeed.
For those who might have missed the beginning of the month’s significant development, Health Secretary Wes Streeting, following a persistent campaign by the Daily Express, committed to offering every cancer patient a personalized cancer plan. This comprehensive plan aims to address various facets of living with cancer, encompassing treatment, mental health, employment, benefits, and more.
To achieve this, medical professionals will need to engage with cancer patients on a deeper level, moving beyond the sterile confines of blood test results. They must see patients as whole individuals, rather than mere medical cases.
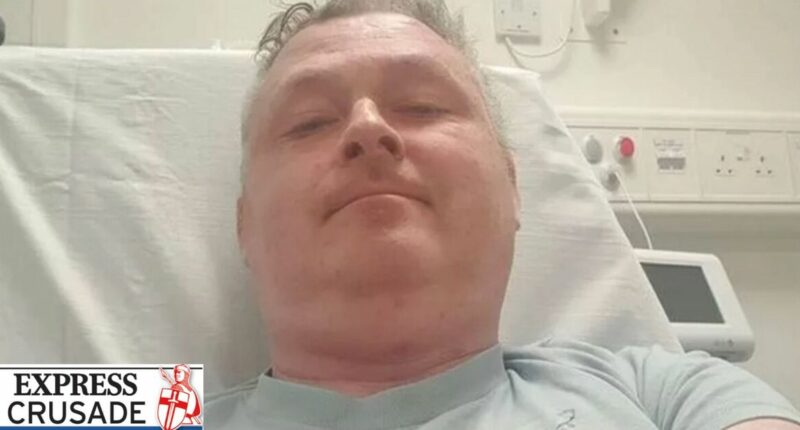
Regrettably, my own experience at a renowned cancer hospital (for context, I am living with incurable bowel cancer) reveals a gap in this approach. However, there is a glimmer of hope on the horizon.
In a recent interaction, a dermatology clinical nurse specialist took a moment to inquire not only about the physical symptoms, such as the cracks in the skin on my hands and the redness on my face, but also asked, “And how are you doing in yourself?”
I was struck by the rarity of such a question and shared with her that she was the first in the entire hospital to ask me about my overall well-being. When I inquired about what actions she would take if I admitted to struggling, she assured me that she would connect me with someone who could offer the necessary support.
She’s asked similar questions before. Not because it’s her job but because she understands that cancer treatment, especially the visual side effects that she’s working to ameliorate, is a mental slog as well as a physical one.
If she gets it then surely other people in cancer hospitals can be trained to get it to?
It made me think of the children’s charity Barnardo’s. They always used to say that children need one trusted adult to tell their problems to.
It’s the same for adults going through cancer treatment. They need at least one trusted adult in their medical team that can be there when the tough times come and keep coming.
In my medical team I really don’t know who that would be. It requires a level of trust that I’m not sure I have in them, even after two-and-a-half years of treatment.
This is why when it comes to any issues I’ll always go and have a chat with my GP. I’m not the only reason why you can’t get an appointment but consultations rarely take less than the 10 minutes I’m told they are supposed to take.
When the personal cancer plans come in I’ll need to establish a similar level of trust with someone in my medical team, with someone who knows how the cancer is slowly destroying me.
It will be a massive challenge for the NHS to shift from asking “How are you?” to asking “How are you?” and it will be a challenge for patients like me too.