Share this @internewscast.com
Nearly half of junior doctors have raised alarms about fatigue-induced clinical mistakes, according to recent findings from the Australian Medical Association (AMA).
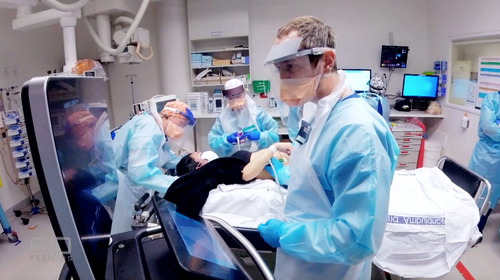
The AMA highlights that exhausted doctors often find themselves assessing patients in emergency rooms after grueling 14-hour shifts.
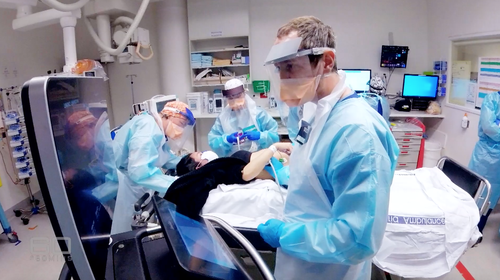
“There’s a risk of prescribing incorrect medication or ordering inappropriate tests,” stated Dr. Simon Judkins, President of AMA Victoria. “None of us want to face such scenarios.”
Dr. Judkins emphasized, “The core of this issue is patient safety. We must ensure that doctors work under conditions that prioritize the well-being of our patients.”
In collaboration with the doctors’ union, the AMA has been negotiating with the Department of Health since August, seeking a new agreement to tackle issues of unsafe scheduling, excessive workloads, and prevalent fatigue.
Doctors are urging the government to implement a cap on shifts, limiting them to 12.5 hours, and to establish restrictions on consecutive night shifts.

They are also asking for a 30 per cent pay rise over four years.
The current EBA is due to expire at the end of April, with doctors not ruling out going on strike as a last resort.
“It’s my expectation that every health service is managing the working conditions of their junior doctors,” Health Minister Mary-Anne Thomas said.
“We have a range of issues for which we’ve got common purpose and we continue to negotiate in good faith.”
But Judkins said the government was still at odds with the association on several points.
“There are still things we need to come to an agreement on,” he said.
“Certainly none of us… want to go down a pathway of industrial action if we can avoid that, but clearly if we can’t find an agreement, that has to be part of our consideration.”
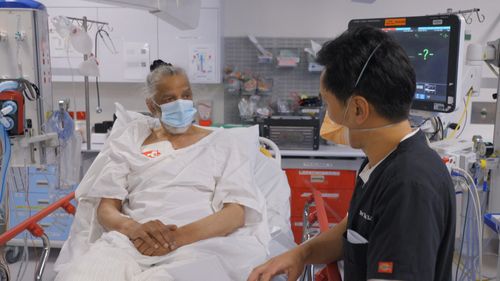
More medical staff could choose to leave the public system if a new EBA wasn’t reached, Judkins warned.
“The danger we have at the moment is people are dropping their hours, they’re going to part-time, they’re dropping out of the public system,” Judkins said.
“We all want a safe system that decreases that stress on our clinicians, gives them a sustainable, long-term career in our public hospital system.”
“We need to come to an agreement on those things because we want those doctors to stay in the public hospital system.”
NEVER MISS A STORY: Get your breaking news and exclusive stories first by following us across all platforms.