Heightened awareness of the potential dangers associated with weight loss drugs has highlighted the urgent need to shift obesity treatment away from a purely medical approach, a prominent expert has cautioned.
Professor Ray O’Connor from the University of Limerick’s School of Medicine raised concerns about the financial viability for the State to cover the costs of so-called “skinny jabs,” especially as geopolitical tensions, like the conflict in Iran, escalate global drug prices.
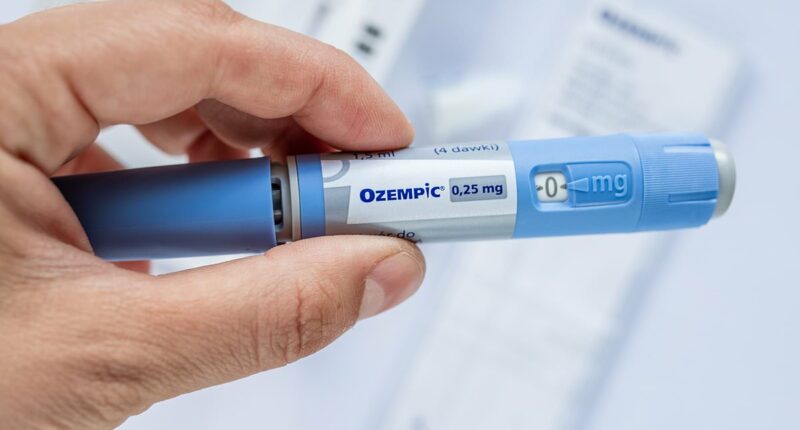
His comments come amid increasing calls for the Government to support the inclusion of GLP-1 weight loss medications, such as Ozempic, Wegovy, and Mounjaro, under the HSE Drug Payment Scheme.
Back in May, Health Minister Jennifer Carroll MacNeill indicated that the Government was considering the option of reimbursing medical card holders for weight loss treatments.
This weekend, however, Prof O’Connor voiced his worries that as more information on the side effects of GLP-1 medications comes to light, it could lead to a misallocation of limited Government resources, potentially detracting from those in greater need.
He explained to the Mail: “The school meals program is costing the State over €200 million annually,” with the Department of Social Protection confirming the expenditure is €288 million.
Then add in a drug payment scheme for these medications to the Budget… and what happens in the case of a recession?’
The Limerick-based GP stressed there are ‘special circumstances and I wouldn’t want to deny anybody who needs’ the weight loss medications.
But he added: ‘We have to give a balanced view, and there are adverse side effects. We have to discuss the State’s ability to pay for its spiralling drug bill. The medications are not free – they are expensive and somebody has got to pay for them.’
The medical practitioner and academic also pointed to growing awareness of the limitations of weight loss medications.
Drugs such as Ozempic have been hailed as miracle treatment but one in 10 people are what scientists call ‘non-responders’.
A major international survey published in January also revealed people who stop taking the jabs return to their original weight in less than two years on average.
And last December the singer Robbie Williams said he feared he may be going blind as a result of taking weight loss drugs.
Prof O’Connor said the side effects experienced by the ex Take That star are ‘rare complications’, adding: ‘Non-arteritic ischemic optic neuropathy, which can affect the optic nerve, can lead to permanent vision loss. It is rare, about one in ten thousand, but when large numbers of people are taking the drug, the cases add up.’

last December the singer Robbie Williams – pictured here with his wife Ayda – said he feared he may be going blind as a result of taking weight loss drugs
Another study found GLP-1 users lose around 16 per cent of their body weight on average within a year of treatment. But Prof O’Connor said expectations can quickly exceed what the medication can deliver, and highlighted other potential side effects.
‘I’ve seen people being very nauseated. I had one patient who was on it, and he was telling me that the nausea would kind of come on every so often, and he was actually in a pool swimming, and he had to get out of the pool to go into the loo to get sick,’ he said.
‘About one in a thousand people per year can develop pancreatitis. If 20,000 people take the drug for a year, that could mean about 20 cases. There are also thyroid tumours at a rate of roughly one in a thousand.’
The health advocate noted that some people taking weight loss drugs simply as a quick fix or to ‘drop a dress size for a wedding’ are not ‘minding what they’re eating in the sense of making sure they have enough protein, doing the weights, so that they preserve body mass and bone mass’.
He also said many GLP-1 users simply ‘get stuck’, and that more must be done to treat the causes, and not just the effects, of the country’s escalating weight problem.
And despite calls on the Government to provide GLP-1s to large numbers of people who cannot afford the drugs, he instead called for the ‘de-medicalisation’ of obesity.
He said: ‘We need to have a proper public health policy on obesity. It’s important to realise that adult obesity rates have more than doubled in the last 35 years since 1990 worldwide.
‘Adolescent obesity has quadrupled. Those are the facts, and there is a lot of discussion about why that is. That’s caused by social factors, not by any genetic issues.

Professor Ray O’Connor of the University of Limerick School of Medicine said the side effects experienced by the former Take That star are ‘rare complications’
‘We also need to look at the whole notion of ultra-processed foods, particularly when it comes to children. If you look at any so-called kiddies’ menus in a restaurant, it’s made up of chips and pizzas and chicken nuggets.
‘We really need to bring dietary nutrition into the national schools particularly. That’s something that I think would be a really important factor in trying to reverse this process.’
Prof O’Connor also called for a national promotional campaign to highlight a more holistic approach to tackling obesity that also educates people around some of the limitations of weight loss medications, saying: ‘It’s to change the narrative around it, that it’s not just a simple jab and all your problems are done.
‘There needs to be monitoring, there are adverse effects, and also that it’s not a case of just taking it for a couple of months or a year, get sorted, and then, you know, Bob’s your uncle.’
Prof O’Connor reiterated he is ‘not against these drugs’ and pointed to ‘some evidence of benefits for kidney disease, cardiovascular disease and possibly conditions like polycystic ovary syndrome’.
But he added: ‘Balance is important. One issue is that these drugs are becoming socially desirable. People are coming in asking for the “skinny jab” so they can drop a dress size or look good in a bikini for the summer.
‘That’s one of the big problems. The conversation around them often doesn’t take into account the potential adverse effects.’
Professor Donal O’Shea, the HSE’s lead on obesity, stressed the positive impact GLP-1s have had on many patients, and noted the drugs have been used safely to treat diabetes for almost two decades.
He agreed ‘anything that causes weight loss can increase frailty if it’s not managed properly’ and said any reimbursement scheme for weight loss drugs should be accompanied with lifestyle programmes.

However, Professor Donal O’Shea, the HSE’s lead on obesity, stressed the positive impact GLP-1s have had on many patients, and noted the drugs have been used safely to treat diabetes for almost two decades.
He told the MoS: ‘We need those programmes to be available digitally. Face-to-face delivery alone is simply too costly at scale.’
Weight loss injections generally cost between €200 and €350-plus per month for private patients.
But Prof O’Shea said he believes costs will fall as patents expire and generic versions become available.
He also stressed the benefits of the medications becoming a routine part of obesity care.
‘It would prevent diabetes and facilitate people accessing treatments like kidney transplantation. The important thing is that obesity is treated as the disease that it is.’
In response to queries, a Department of Health spokesperson said the HSE’s leadership decides, ‘based on all competing demands across the health service, whether a new medicine, or a new use of an existing medicine, can be funded within the resources available, in line with the legislation’.
They added that Liraglutide (Saxenda) was the only GLP-1 currently reimbursed for managing weight-loss by the HSE.