Share this @internewscast.com
Last October, I embarked on what was supposed to be an unforgettable cruise to the Virgin Islands. However, the trip took a terrifying turn when I woke up in the dead of night, gripped by a pain so severe that I feared I might be suffering a heart attack.
Sweat-drenched and in a state of panic, I managed to make my way to the ship’s medical center. The on-board doctor examined me, and when she pressed on the upper right side of my abdomen, a sharp pain elicited a scream that echoed through the corridors. Her diagnosis was clear: an inflamed gallbladder.
In my panic, I couldn’t help but turn to the internet for answers. What I found left me nauseated with fear. An inflamed gallbladder, I read, could rupture, a potentially fatal condition. Being miles away from the nearest hospital, stranded in the vast Caribbean Sea, only amplified my anxiety. The thought of not returning to my four-year-old daughter, of her growing up without her mother, was a haunting specter I couldn’t shake.
Back on land in London, a consultant gastroenterologist confirmed my fears. He suggested that my condition could have been self-inflicted. Like 1.6 million others in the UK, I had been using weight-loss injections, a decision that now seemed to have dire consequences.
Far from a hospital, in the middle of the Caribbean Sea, this would be a scary prospect for anyone. The thought of leaving my four-year-old daughter without a mum, if anything should go wrong, was utterly unbearable.
Worse still, I feared – something later backed up by a consultant gastroenterologist back home in London – that I had brought this on myself. You see, like 1.6million others in the UK, I had been using weight-loss injections.
While I can’t definitively prove the link in my case, surgeon Ahmed Ahmed, president of the British Obesity and Metabolic Specialist Society, said this year that there appears to be a connection between use of the jabs and the risk of developing gallstones.
He reported that ‘more and more’ of those coming to him for gallbladder operations were saying they had used GLP-1 receptor agonists (GLP-1s), including Wegovy, Ozempic and Mounjaro. Indeed, Mounjaro manufacturer Eli Lilly now cites gallbladder infection as a potential, if uncommon, side-effect.

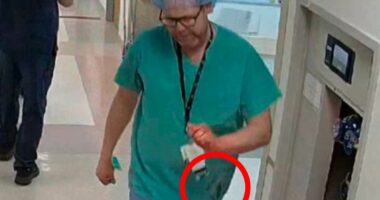
Lynn Carratt was on a cruise ship in the middle of the Carribbean Sea when she woke up in so much pain she was convinced she was having a heart attack
In addition, NHS England figures show that, between 2024 and 2025, at a time when the popularity of fat jabs was ballooning, the number of gallbladder surgeries was at its highest peak in a decade.
The risk comes because GLP-1s slow down the emptying of the gallbladder, which stores and releases bile to help with the absorption and digestion of fats.
Additionally, losing weight quickly causes the liver to release extra cholesterol into the bile, which can also lead to gallstone formation.
I barely slept a wink after my gallbladder issues were diagnosed. We were several days away from the nearest hospital so I faced an agonising wait for the all-important scan that would assess the extent of the inflammation. I had plenty of time to dwell on my foolish decision to resort to Mounjaro.
As a journalist and publicist, I’d read so many positive stories of people whose bodies, lives even, had been transformed by the jabs. Naturally, I was very much looking forward to having this helping hand in my own battle with the flab.
So, in February last year, at the age of 43, I had an assessment at my local pharmacy. At 14st 7lbs and 5ft 2ins tall, giving me a BMI of 37, I was classed as obese and prescribed a month’s worth of Mounjaro, at the starting dose of 2.5mg.
My weight has always fluctuated. I’ve been everything from 15st to 8st 7lbs since my late teens and tried every diet under the sun.
However, after having my daughter, Mia, I just couldn’t seem to get rid of the excess weight I’d gained during pregnancy, a fact exacerbated by lack of sleep and time, which meant my husband James and I spent far too many evenings at home in east London eating ready meals.
Blood tests arranged by my GP had shown I had fatty liver disease, which is linked to obesity, as well as metabolic syndrome – the symptoms of which are high blood pressure and high blood sugar – which can lead to cardiovascular disease and type 2 diabetes.
Both of these conditions can be reversed by losing weight and so I decided fat jabs were the answer to my prayers.
I read the potential side-effects and carefully weighed them up. I fully expected a bit of temporary fatigue and nausea and I was also made aware of the pancreatitis risk, but felt reassured that the likelihood was very small. I don’t remember any mention of the gallbladder, though.
My weight loss journey was tough from the start. For the first four weeks, I felt constantly nauseous, even vomiting on a few occasions, and also experienced stomach ache and diarrhoea.
However, by the end of February, I’d lost half a stone, which was so heartening I did a second month on the 2.5mg dose.

A trip to the ship’s medical centre showed that she had an inflamed gallbladder – which can affect up to one in 100 people taking weight-loss jabs such as Mounjaro

I’d read so many positive stories of people whose bodies, lives even, had been transformed by the jabs, writes Lynn. Naturally, I was very much looking forward to having this helping hand
By then, my body must have adjusted, as I had no unpleasant side effects in March, and lost another half stone.
However, come April, when I increased my dose to 5mg, I felt permanently exhausted.
My GP recommended vitamin B12 injections, after tests showed I was deficient, but, even then, the fatigue never dissipated.
So, after another month on a 5mg dose, I decided to go back down to 2.5mg in July, by which time I’d lost a total of two stone.
Perhaps my body had adapted, but, after that, I lost no more weight, which was disheartening, as I was still two stone away from having a healthy BMI.
Come September, I decided not to waste another £175 – the 5mg dose cost £200 a month – and didn’t buy another pen.
Little did I know what damage I might already have done.
It was mid-September when I first started feeling pain in my lower abdomen, which was more intense when I’d eaten fatty food or drank alcohol.
At this stage, I put it down to digestive problems and took Rennies and Buscopan, an antispasmodic, as I also suffer from irritable bowel syndrome.
The discomfort mostly came at night, making it difficult to sleep. However, it wasn’t serious enough for me to even consider not heading to New York with James, 44, and Mia at the beginning of October, from where we set sail on our cruise around the Virgin Islands.
Having continued to ignore the niggling discomfort, we were a week into our three-week trip when I woke in the night in so much pain, in my chest and abdomen, I thought I was having a heart attack.
Clutching my torso, I told my husband there must be something seriously wrong and that I was going to get checked out at the medical centre.
I’m sure he thought I was exaggerating – he knows I’m prone to health anxiety – so didn’t say much, other than that he would stay in our cabin with Mia who was still asleep.
The doctor examined me and, hearing my screams when she pressed my abdomen, said: ‘Oh, I think you’ve got an inflamed gallbladder.’
As inflammation is usually caused by bile trapped by gallstones which, in turn, can lead to bacterial infections, she hooked me straight up to a drip and administered intravenous antibiotics.
She also gave me anti-inflammatory and antibiotic tablets, to take regularly throughout the day.
Although I had health insurance, I had to pay for my treatment upfront – a total of £1,000 over five days – before claiming back most of it, minus the £350 excess, once we were home.
James brought Mia to visit me when she woke up. Seeing me pale, sweating and wired up to a drip, she looked so worried, giving me a kiss and saying: ‘Get better soon, Mummy.’ I told her: ‘Mummy is just sick this morning, but she’ll be better this afternoon.’
Really, I was trying to reassure us both.
All I could think was, what if something serious happens to me, just because I used weight loss jabs, and Mia loses her mum?

Every morning on the cruise Lynn was given a hefty dose of intravenous antibiotics for about an hour

This experience has taught me there’s no shortcut to health, and that weight-loss jabs are not the magic solution everyone thinks they are, says Lynn
She spent a lot of time over the coming days in the kids’ club, which was not what we’d planned for our family trip of a lifetime, but it proved a great distraction.
The doctor said I urgently needed an ultrasound scan. We stopped at St Croix the following day and St Kitts the day after that but, because it was a weekend, neither of their radiology departments was open.
Then we docked in St Martin on the Monday, but, to my dismay, we had arrived on a bank holiday, meaning there were no radiologists on duty there either.
So, each morning, the on-board doctor would hook me up and administer another hefty dose of intravenous antibiotics and then send me on my way, with a fistful of oral antibiotics and anti-inflammatories.
The sessions lasted about an hour, and afterwards I would lie down for 30 minutes in the on-board hospital, before heading back to the cabin to rest.
I could eat small meals, but with an inflamed gallbladder I had to avoid anything fried, greasy, or containing full-fat or refined sugars. This was particularly challenging on an American ship.
Feeling sick and exhausted, and still experiencing a lot of abdominal pain, I still tried to get out and see some of the sights, mostly for Mia’s sake.
I really didn’t want her worrying about me so, while trying to suppress my own terror that my gallbladder could rupture any minute, we built sandcastles and paddled in the clear Caribbean Sea.
Finally, in Tortola, the largest of the Virgin Islands, where we docked on the Tuesday, I was able to have an ultrasound scan, at an additional cost of £500.
It showed that, thanks to the medication I’d been taking, the inflammation was going down; however, the wall of my gallbladder was still thicker than it should have been.
The hospital doctor recommended I keep taking the pills and have another scan once back in the UK.
The antibiotics and painkillers had started working after about 48 hours, and I began to feel better as the inflammation in my gallbladder settled. However, the fatigue lingered for much longer, even after we returned home.
At the end of October, a week after we got home, I had an appointment with a consultant gastroenterologist.
He ordered a CT scan which showed the gallbladder wall was thickened but no longer inflamed and referred me for an MRI scan.
This revealed three small bodies, either gallstones or polyps which could only be eliminated through removal of the gallbladder.
However, as I was no longer in pain I didn’t want to risk an operation, under general anaesthetic – something I’ve never had before – so have instead opted for a watch and wait approach which involves regular scans.
Touch wood, I haven’t had any issues with my gallbladder since New Year’s Day but I may potentially require surgery in the future.
My consultant told me that, while he couldn’t say with absolute certainty, he thinks it’s ‘likely’ taking Mounjaro caused my gallbladder to become inflamed.
So, for the past three months I’ve concentrated on losing weight naturally, reducing fat and alcohol and increasing my intake of vegetables and fibre, as well as taking up reformer Pilates.
This experience has taught me there’s no shortcut to health, and that weight-loss jabs are not the magic solution everyone thinks they are.
Now my advice to anyone taking them is to be alert to any physical signs that they could be doing serious harm and, if you have concerns, seek immediate medical attention.
A spokesman for Eli Lilly said: ‘Patient safety is Lilly’s top priority and we actively monitor, evaluate, and report safety information for all our medicines to the MHRA. The Mounjaro (tirzepatide) Patient Information Leaflet warns that cholecystitis (infection of the gallbladder) is an uncommon side effect, which may affect up to one in 100 people.
‘Anyone experiencing side effects when taking any Lilly medicine should consult their doctor or other healthcare professional, and should ensure that they are getting genuine Lilly medicine.’