Share this @internewscast.com
A group of experts tasked by the World Health Organization to investigate how the COVID-19 pandemic began has released its final report. It shows that scientists still aren’t sure how the worst health emergency in a century started.
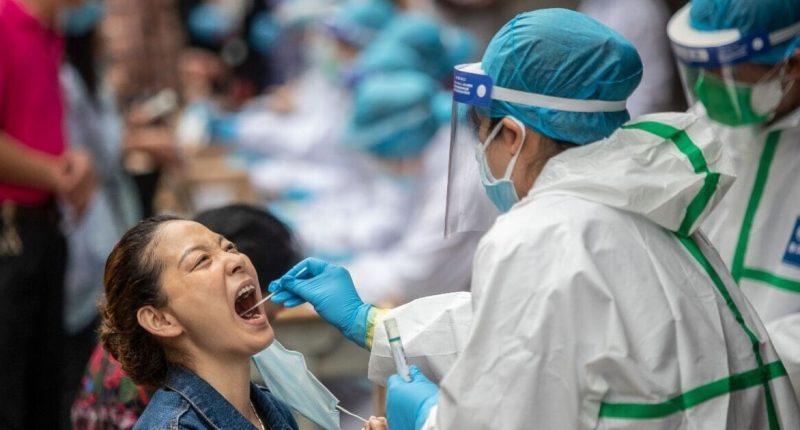
Professor Marietjie Venter, who chairs the group, said on Friday (June 27) that most scientific data supports the idea that Covid jumped from animals to humans. It is the same conclusion drawn by the first WHO expert group, which investigated the pandemic’s origins in 2021.
Scientists then concluded the virus was likely to have spread from bats to humans, via another animal. At that time, the WHO said a lab leak was “extremely unlikely”.
Ms Venter said after more than three years of work, WHO’s expert group was unable to get the data it needed to evaluate whether or not COVID-19 was the result of a lab accident.
This was despite repeated requests for hundreds of genetic sequences and more detailed biosecurity information sent to the Chinese government.
She said: “Therefore, this hypothesis could not be investigated or excluded. It was deemed to be very speculative, based on political opinions and not backed up by science.”
The professor also said the group’s 27 members failed to reach a consensus. One member resigned earlier this week while three others asked for their names to be removed from the report.
Ms Venter said there was no evidence to prove COVID-19 had been manipulated in a lab, nor was there any indication the virus had been spreading before December 2019 anywhere outside of China.
Referring to the scientific name for COVID-19, she said: “Until more scientific data becomes available, the origins of how SARS-CoV-2 entered human populations will remain inconclusive.”
WHO Director-General Tedros Adhanom Ghebreyesus said it was a moral imperative to determine how Covid began, noting the virus killed at least 20 million people worldwide, wiped at least £7.3trillion ($10tn) from the global economy and upended billions of lives.
It emerged in 2024 that Beijing froze meaningful domestic and international efforts to trace the origins of the virus in the first weeks of the outbreak in 2020 and that the WHO itself may have missed early opportunities to investigate how COVID-19 began.
US President Donald Trump has long blamed the emergence of the coronavirus on a laboratory accident in China, while a US intelligence analysis found there was insufficient evidence to prove the theory.
Chinese officials have repeatedly dismissed the idea the pandemic could have started in a lab, saying the search for its origins should be conducted in other countries.
Last September, researchers zeroed in on a shortlist of animals they believed may have spread COVID-19 to humans, including racoon dogs, civet cats and bamboo rats.