Share this @internewscast.com
If you’re trying to lose fat around your belly and looking for healthy, nutrient-dense meals, we’ve got you covered. We aren’t here to tell anyone they need to lose this fat, but if you’ve decided to go on this journey yourself, we can help by providing some delicious belly fat-burning meals you’ll want to make a part of your routine.
What exactly gives a meal “belly fat-burning” qualities? There are a few key things to consider when deciding on meals that fit your weight loss goals. Ultimately, what matters is what fits into your personal needs, but the following characteristics are a good place to start:
- High in protein: Eating enough protein at meals ensures that you’ll feel full, can improve your metabolism, and can help you burn fat and build lean muscle. Studies show that eating a high-protein diet can directly help with abdominal fat loss.
- Contains fiber: Foods with fiber can help you burn belly fat because fiber can increase satiety, improve digestion, and even help you have a healthier gut—something that has recently been linked to weight loss. Research has shown that eating more fiber can help prevent weight gain around your abdominal area.
- Has healthy fats: Foods with healthy fats (think olive oil, fish, nuts, seeds, avocado, etc.) have been linked to increased weight loss because of their ability to improve satiety and burn fat—specifically around the abdomen.
For some inspiration about healthy meals that meet one or more of these qualities, we’ve gathered 25 belly fat-burning recipes that you can try today. Read on, then check out the 25 Best-Ever Fat-Burning Foods.
Hearty Turkey Chili

Nutrition (Per serving):
Calories: 330
Fat: 6 g (Saturated Fat: 1 g)
Sodium: 490 mg
This chili has everything you’d want and need from a belly fat-burning meal. Full of protein and fiber and low in calories, you’ll enjoy every bite and will feel full until your next meal. Top with your favorite chili ingredients like shredded cheese, sour cream, and scallions.
Get our recipe for Hearty Turkey Chili.
Black Bean Omelet

Nutrition (Per serving):
Calories: 330
Fat: 8 g (Saturated Fat: 6 g)
Sodium: 480 mg
Starting your day with a high-protein, high-fiber breakfast is a helpful way to burn fat and stay full until lunchtime. Not only is this omelet full of helpful nutrients, but it’s super easy to make so you won’t have to put in too much effort first thing in the morning.
Get our recipe for Black Bean Omelet.
Slow Cooker Green Chile Pork Soup

Nutrition (Per serving):
Calories: 359
Fat: 3 g (Saturated Fat: 1 g)
Sodium: 667 mg
Sugar: 5 g
Fiber: 6 g
Protein: 25 g
Soup is a healthy weight-loss food because it’s often lower in calories and allows you to pack in a ton of nutrients. This Green Chile Pork Soup is a great example, as it’s full of protein and fiber from pork, beans, potatoes, chiles, onion, poblano peppers, and Greek yogurt.
Get the recipe for Green Chile Pork Soup.
Grilled Mahi-Mahi with Salsa Verde

Nutrition (Per serving):
Calories: 280
Fat: 15 g (Saturated Fat: 2.5 g)
Sodium: 390 mg
When you’re looking for a fat-burning food, don’t forget about fish! Fish has healthy fats and protein that can keep you full and support your weight loss goals, and this Mahi-Mahi recipe is a delicious way to enjoy more fish in your diet.
Get our recipe for Grilled Mahi-Mahi with Salsa Verde.
Greek Salad Recipe with Chicken

Nutrition (Per serving):
Calories: 360
Fat: 22 g (Saturated Fat: 7 g)
Sodium: 580 mg
Healthy meals that you can throw together in a matter of minutes are the best recipes for weight loss because you can rely on having nutritious food even on your busiest days. This Greek Salad with Chicken is exactly that, and all you have to do to make it is combine the chicken, bell peppers, cucumbers, tomatoes, garbanzo beans, feta cheese, and seasonings. Because of the chicken, vegetables, and garbanzo, this meal has plenty of helpful protein and fiber to keep you full.
Get our recipe for Greek Salad Recipe with Chicken.
Grilled Pork Tenderloin with Pineapple Salsa
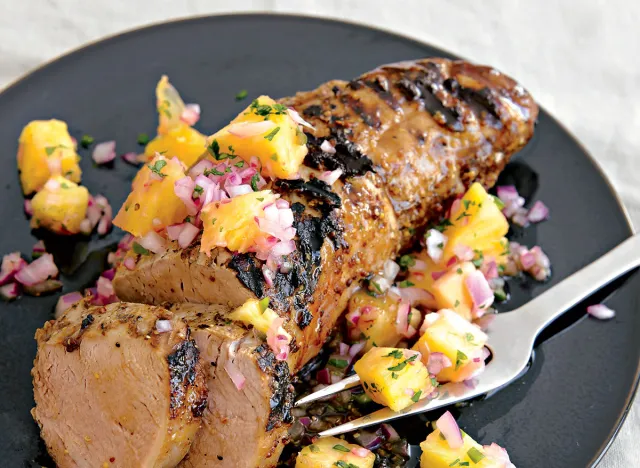
Nutrition (Per serving):
Calories: 210
Fat: 4 g (Saturated Fat: 1.5 g)
Sodium: 390 mg
People usually think of chicken and turkey when they think of lean protein, but don’t forget about pork tenderloin. This lean cut of pork has very little fat (2.5 grams) and contains a ton of protein (24 grams) per serving, making it a great ingredient in your belly fat-burning meals. Combine with a tasty pineapple salsa and you have a flavorful, nutritious lunch or dinner.
Get our recipe for Grilled Pork Tenderloin with Pineapple Salsa.
Vegetable Quinoa Soup

Nutrition (Per serving):
Calories: 304
Fat: 9.5 g (Saturated Fat: 1.5 g)
Sodium: 703 mg
Quinoa is a grain that contains high amounts of both protein and fiber, so it’s the perfect foundation for healthy meals. This Vegetable Quinoa Soup is simple and uses only quinoa, carrots, celery, vegetable broth, garlic, and seasonings, and if you want to add even more protein, you can throw in some chicken or ground turkey. Want more fiber and healthy fats, add some diced avocado on the top.
Get the recipe for Vegetable Quinoa Soup.
Moroccan-Inspired Quinoa Pilaf and Salmon

Nutrition (Per serving):
Calories: 310
Fat: 13 g (Saturated Fat: 2 g)
Sodium: 780 mg
When you find a meal that contains protein, fiber, and healthy fats, you’ve found a fat-burning winner. Protein from the quinoa and salmon, fiber from the quinoa and raisins, and healthy fats from the salmon and pine nuts mean you can’t go wrong with this fish recipe.
Get our recipe for Moroccan-Inspired Quinoa Pilaf and Salmon.
Sunrise Sandwich

Nutrition (Per serving):
Calories: 380
Fat: 13 g (Saturated Fat: 3.5 g)
Sodium: 980 mg
Fans of a classic egg breakfast sandwich will love this Sunrise Sandwich, which is an English muffin piled high with egg, smoked turkey, cheese, tomato, and avocado. The combination of protein, fiber, and healthy fats ensures that you won’t feel hungry afterward, and for only 380 calories, this is a no-brainer.
Get our recipe for Sunrise Sandwich.
Chicken Burger with Sun-Dried Tomato Aioli

Nutrition (Per serving):
Calories: 330
Fat: 14 g (Saturated Fat: 3 g)
Sodium: 730 mg
Opting for a chicken burger over a regular beef burger means you can still enjoy the same high-protein content but with much less total fat and saturated fat. However, chicken burgers can sometimes have less flavor than beef. Thankfully that’s not the case with these chicken burgers topped with a homemade sun-dried tomato aioli. Eat over a bed of lettuce if you’re trying to eat low-carb, or enjoy with your favorite whole-wheat bun for added fiber.
Get our recipe for Chicken Burgers with Sun-Dried Tomato Aioli.
Healthier Grilled Caesar Salad

Nutrition (Per serving):
Calories: 410
Fat: 29 g (Saturated Fat: 3.5 g)
Sodium: 610 mg
People may assume that they can’t enjoy creamy salad dressings if they’re watching their calorie intake, but this isn’t always the case. When you make a homemade Caesar dressing, you can control how much mayo you use, which means you can cut down on calories from fat. This Caesar salad also includes chicken for protein, so it’s a win-win!
Get our recipe for Healthier Grilled Caesar Salad.
Baked Chicken with Tomatoes and Capers

Nutrition (Per serving):
Calories: 310
Fat: 18 g (Saturated Fat: 2.5 g)
Sodium: 420 mg
Chicken is a wonderfully versatile lean protein to use in your weight loss plans, but it’s easy to grow tired of the same chicken dishes. If you need a new way to enjoy chicken, try this baked chicken with capers, tomatoes, onions, olives, pine nuts, and basil.
Get our recipe for Baked Chicken with Tomatoes and Capers.
Teriyaki Pork Chops with Sauteed Apples

Nutrition (Per serving):
Calories: 315
Fat: 9 g (Saturated Fat: 3.5 g)
Sodium: 890 mg
These pork chops are a simple and delicious way to meet your protein needs for the day, and they use simple ingredients to bring out a ton of flavor. Serve with a salad or your favorite vegetables to get in some extra fiber and nutrients.
Get our recipe for Teriyaki Pork Chops with Sauteed Apples.
Chicken Cacciatore

Nutrition (Per serving):
Calories: 430
Fat: 13 g (Saturated Fat: 2 g)
Sodium: 560 mg
This classic Italian-American dish gets most of its powerful flavors from vegetables and fruits, so it’s easy to keep the calories on the lower end. Made with chicken, tomatoes, garlic, olives, bell peppers, parsley, and dry red wine, you’ll love this healthy chicken dish and will want to make it a part of your routine.
Get our recipe for Chicken Cacciatore.
Instant Pot Shrimp and Broccoli

Exact nutrition information is not available.
Instead of ordering takeout, try your hand at this shrimp and broccoli recipe yourself, which you can make in the Instant Pot to save time and effort. Full of ingredients that are rich in fiber and protein, this meal will leave you feeling satisfied every time.
Get our recipe for Instant Pot Shrimp and Broccoli.
Chicken Mole Enchiladas

Nutrition (Per serving):
Calories: 410
Fat: 15 g (Saturated Fat: 3.5 g)
Sodium: 430 mg
Need an easy, high-protein meal for lunch or dinner? These mole enchiladas are the perfect recipe. Not only will you get protein to help meet your goals for the day, but you can use leftover rotisserie chicken, which means you barely have to cook anything at all.
Get our recipe for Chicken Mole Enchiladas.
Healthy Chicken Tikka Masala

Nutrition (Per serving):
Calories: 280
Fat: 10 g (Saturated Fat: 3 g)
Sodium: 824 mg
Carbohydrates: 20 g (Fiber: 4 g, Sugar: 2 g)
Protein: 32 g
If you’re craving Tikka Masala but want more control over the ingredients you consume, try making your own instead of ordering takeout. With ingredients like Greek yogurt, chicken, and half and half, you’ll get plenty of protein. Another plus is that you’ll also get 4 grams of filling fiber, too.
Get our recipe for Healthy Chicken Tikka Masala.
Protein Pancakes

Exact nutrition information is unavailable.
What better way to increase your protein intake than with pancakes? This recipe uses protein powder, Greek yogurt, milk, and oats to make hearty, filling pancakes. Want to up the flavor more? Try using a chocolate protein powder or other flavor of your choosing!
Get our recipe for Protein Pancakes.
Spanish Garlic Shrimp

Nutrition (Per serving):
Calories: 250
Fat: 15 g (Saturated Fat: 2 g)
Sodium: 310 mg
Make this simple shrimp dish and enjoy protein and healthy fats to help keep you full until your next meal. You can pair it with a salad, some vegetables, rice, or your favorite whole-wheat pasta for added fiber.
Get our recipe for Spanish Garlic Shrimp.
Pumpkin Mole Chili

Nutrition (Per serving):
Calories: 265
Fat: 7 g (Saturated Fat: 2 g)
Sodium: 450 mg
Fiber: 8 g
Sugar: 10 g
Protein: 23 g
This Pumpkin Mole Chili has it all. Protein from the ground beef, beans, and Greek yogurt, fiber from the pumpkin, beans, and veggies, and healthy fats from the canned pumpkin. This dish is full of flavor and makes for the perfect meal to melt away belly fat.
Get our recipe for Pumpkin Mole Chili.
Paleo Turkey Bolognese with Garlic Spaghetti Squash

Nutrition (Per serving):
Calories: 370
Fat: 9 g (Saturated Fat: 3 g)
Sodium: 790 mg
Fiber: 8 g
Sugar: 6 g
Protein: 22 g
If you’re following the Paleo diet and miss your favorite pasta dishes, this Spaghetti Squash Bolognese is a tasty alternative. But you don’t have to be following a Paleo eating plan to enjoy this one, as it’s also perfect for those wanting to lower their fat or carbohydrate intake.
Get our recipe for Paleo Turkey Bolognese with Garlic Spaghetti Squash.
Minestrone Soup with Pesto

Nutrition (Per serving):
Calories: 200
Fat: 5 g (Saturated Fat: 1.5 g)
Sodium: 490 mg
For a soup that’s going to give you that necessary fiber to keep you full and give you a healthy gut, we love this Minestrone Soup with Pesto. It’s easy to make, and you can make a larger batch and save to heat up throughout the week, which will help you when you want a healthy meal on busy days.
Get our recipe for Minestrone Soup with Pesto.
Oatmeal With Peanut Butter and Banana

Nutrition (Per serving):
Calories: 320
Fat: 10 g (Saturated Fat: 1 g)
Sugar: 17 g
This oatmeal recipe is a healthy weight-loss breakfast for those who love something on the sweeter side in the morning. Packed with peanut butter, nuts, and bananas, you’ll enjoy comforting flavors while getting protein, fiber, and healthy fats.
Get our recipe for Oatmeal With Peanut Butter and Banana.
Breakfast Hash with Sweet Potato and Chicken Sausage

Nutrition (Per serving):
Calories: 230
Fat: 11 g (Saturated Fat: 4.5 g)
Sodium: 290 mg
Now for the savory breakfast lovers. This breakfast hash made with sweet potatoes, chicken sausage, and eggs will fill you up and give you a fat-burning boost first thing in the morning.
Get our recipe for Breakfast Hash with Sweet Potato and Chicken Sausage.
Spicy-Sweet Grilled Chicken Pineapple Sandwich

Nutrition (Per serving):
Calories: 400
Fat: 11 g (Saturated Fat: 6 g)
Sodium: 640 mg
If you’re a fan of a spicy-sweet combo, this sandwich is for you. It’s grilled, so you can avoid the excess calories and fat that come from a fried chicken sandwich, but this recipe is still just as satisfying. Enjoy protein from the chicken and for added fiber, use a whole-wheat bun!
Get our recipe for Spicy-Sweet Grilled Chicken Pineapple Sandwich.












