Share this @internewscast.com

SEOUL — On Sunday, North Korea executed a fresh round of tests involving strategic cruise missiles and anti-warship missiles, as part of ongoing assessments of the destroyer Choe Hyon’s operational capabilities, according to the state news agency KCNA on Tuesday.
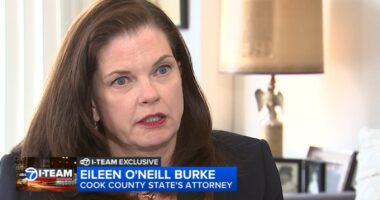
Leader Kim Jong Un supervised the missile tests, accompanied by top defense officials and naval commanders, as detailed in the report.
The operation included the launch of two strategic cruise missiles and three anti-warship missiles. The objectives were to evaluate the warship’s integrated weapons command system, train the crew in missile launch protocols, and confirm the precision and anti-jamming capabilities of its upgraded navigation systems, as per KCNA.
The cruise missiles traveled for durations ranging from approximately 7,869 to 7,920 seconds, while the anti-warship missiles were airborne for about 1,960 to 1,973 seconds. All missiles struck their targets with what the report described as exceptional precision over the waters off the nation’s western coast.
On the same day, Kim received updates on the development of weapons systems for two additional destroyers currently in the construction phase, signaling plans for the third and fourth vessels in the Choe Hyon series.
Kim emphasized the importance of bolstering North Korea’s nuclear deterrence capabilities, highlighting the need to enhance both strategic and tactical strike abilities as well as rapid-response readiness, as noted in the report.
Pyongyang first test-fired weapons on the 5,000-ton Choe Hyon-class warship in April 2025, and in June, Kim announced plans to build two additional destroyers in 2026 and commission two ships of the same or a more advanced class annually.
Lim Eul-chul, a professor at Kyungnam University, said the reference to a fourth destroyer appeared to be the first official acknowledgment of construction on the vessel beyond earlier announcements.
“The mention of the third and fourth destroyers suggests North Korea is accelerating the formation of a destroyer flotilla rather than fielding isolated platforms,” Lim said, adding that faster follow-on production typically follows once initial testing is deemed successful.
Lim said weapons development appeared to be speeding up across multiple fronts as North Korea seeks to exploit global strategic distractions, including the conflict in the Middle East, to push ahead with irreversible advances in nuclear and delivery capabilities.
The North Korean embassy in Beijing did not immediately respond to a request for comment.