Share this @internewscast.com
The innovative BRAIx tool, developed in Australia, offers a groundbreaking approach to breast cancer detection. This predictive technology is designed to analyze mammogram images to not only identify existing cancer but also to forecast the potential development of the disease within a four-year timeframe for Australian women.
Traditionally, mammogram evaluations involve two radiologists, with a third brought in if their assessments differ. The BRAIx tool adds a sophisticated layer to this process, employing advanced algorithms to scrutinize the same images for signs or risks of cancer, enhancing the overall accuracy of these screenings.

Far from replacing the expertise of radiologists, this AI tool acts as an invaluable assistant. It enhances the precision and efficiency of breast screenings, according to researchers involved in its development.
Dr. Helen Frazer, the clinical director of St Vincent’s Breast Screen, highlighted the tool’s capability to recognize early cancer signs or risk patterns that might elude the human eye. “Our algorithm has been trained on millions of mammogram images, vastly exceeding what any radiologist could review over their career,” Frazer explained.
This extensive training, based on real mammogram images from Australia’s national screening program, positions BRAIx as a cutting-edge asset in the fight against breast cancer, significantly aiding radiologists in their critical work.
“We’ve been able to train the algorithm on millions of mammogram images, many more than a radiologist would ever be able to see in their lifetime,” Frazer said.
“It’s using simple image classification algorithms to detect signs of cancer or the risk of cancer on a mammogram.
“We can create really accurate tools that have been trained on local Australian populations to improve the population screening program for Australian women.”
The BRAIx detection tool is currently being used in a randomised controlled trial at Breast Screen Victoria and is soon to be rolled out at Breast Screen SA.
The technology has expanded to generate risk scores, predicting a patient’s likelihood of developing breast cancer within the next four years.
The risk-prediction tool is in research and development, Frazer said.
“This is an Australian first for an AI, high-consequence decisions in health care,” she said.
“This will provide us with the necessary evidence for trusts in AI tools for high-consequence healthcare decisions.”
Currently, doctors analyse age, family history and breast density to determine the risk of developing breast cancer.
But research shows the BRAIx tool can predict cancer “with much greater accuracy” than ever before.
“One in 10 women that had a BRAIx risk score in the top two per cent of the population cohort that we tested went on to develop breast cancer in the next four years,” Frazer said.
“And they had been given an all-clear at [mammogram] screening.”
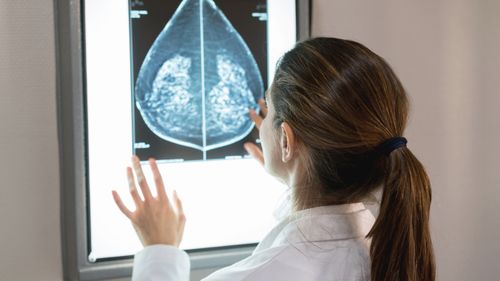
“That really is a breakthrough finding… the future for AI-leveraged risk detection is incredibly exciting.”
The tool could mean the most significant “quantum change” in breast cancer deaths in Australia since the national breast cancer screening program was introduced for women over 50 more than 30 years ago.
Despite the introduction of the screening program, 90,000 Australian women are expected to die from breast cancer in the next 25 years.
Frazer hopes the Australian-built tool can put a stop to the sobering statistic.
“What we’ve learned from the screening program is that if we detect cancer early, whilst it’s still in the breast and hasn’t spread to lymph nodes or distant organs, we have an almost perfect survival [rate] with modern-day treatments,” she said.
“If we can make it even more accurate, detect cancer even earlier, and actively invite women at age 40, and maybe in the future at an even younger age, we have the potential to detect every woman’s cancer early and save every woman’s life.”
NEVER MISS A STORY: Get your breaking news and exclusive stories first by following us across all platforms.













